Root Canal
Procedure
Endodontic Microsurgery
“Root Canal” (Endodontic) Therapy
Root canal (endodontic) treatment is necessary when the pulp becomes inflamed or infected. The most common causes of inflammation or infection are deep cavities (caries), cracks or chips, repeated dental procedures, or even dental trauma. If pulp inflammation or infection is left untreated, it can cause pain or lead to an abscess. Root canal treatment is an alternative to extraction of a tooth, relieving discomfort and allowing you to maintain your natural tooth.
A root canal procedure to remove the pulp tissue is usually performed over several visits by a regular dentist or a pulp specialist, called an endodontist. The goal of root canal therapy is to spare you from having to get the infected tooth removed. It’s always better to have your natural teeth when possible!
What is Root Canal Treatment?
Root canal (endodontic) treatment is performed under a local anesthetic to eliminate discomfort during the procedure. The doctor takes special care to remove the injured and/or diseased pulp. The root canal system is then thoroughly cleaned and sealed with a specialized root filling.
Root canal treatment can often be completed in one visit but sometimes several visits are needed. Back teeth usually require more time for treatment because they have more canals and are harder to reach.
What to Expect from Root Canal Therapy
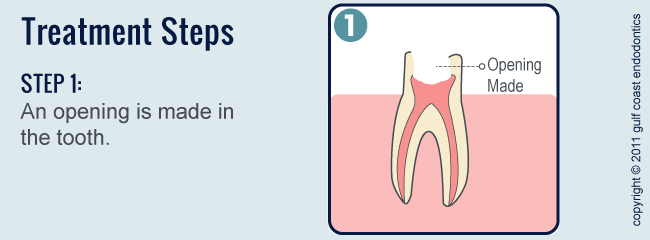
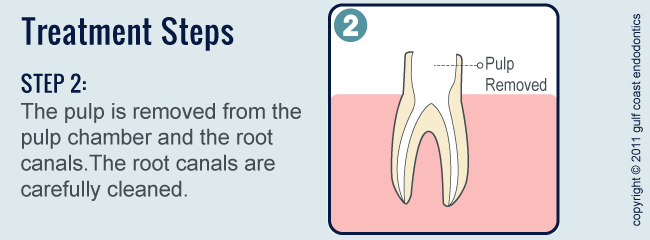
- First visit. The diseased pulp is removed and the empty space, the root canal, is cleaned out and enlarged. Special medications may be placed in the canal to disinfect the area. A temporary filling may be placed as well, or your dentist may choose to leave the canal open and let the tooth drain for a few days. An oral antibiotic may also be recommended to treat infection in the tissues surrounding your tooth.
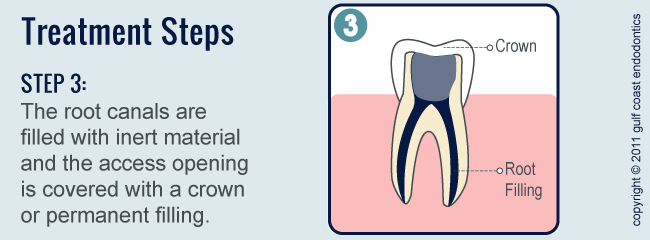
- Second visit. The temporary filling is removed and a permanent filling is placed.
- Final visit. A crown is placed over the tooth to reinforce the tooth and make it stronger.
Root Canal Benefits
Root canal (endodontic) treatment saves teeth that would otherwise be extracted. Although the pulp has been removed, the tooth is still anchored in the bone and can still be used for biting and chewing. With proper care, most teeth that have had root canal treatment can last as long as other natural teeth!
Endodontic Basics
Can all teeth be treated endodontically?
Most teeth can be treated. Occasionally, a tooth can’t be saved because the root canals are not accessible, the root is severely fractured, the tooth doesn’t have adequate bone support, or the tooth cannot be restored. However, advances in endodontics are making it possible to save teeth that even a few years ago would have been lost. When endodontic treatment is not effective, endodontic surgery may be able to save the tooth.
What are the signs of needing endodontic treatment?
Signs to look for include pain, prolonged sensitivity to heat or cold, tenderness to touch and chewing, discoloration of the tooth, and swelling, drainage and tenderness in the lymph nodes as well as nearby bone and gingival tissues. Sometimes, however, there are no symptoms.
Why would I need an endodontic procedure?
Endodontic treatment is necessary when the pulp, the soft tissue inside the root canal, becomes inflamed or infected. The inflammation or infection can have a variety of causes: deep decay, repeated dental procedures on the tooth, or a crack or chip in the tooth. In addition, an injury to a tooth may cause pulp damage even if the tooth has no visible chips or cracks. If pulp inflammation or infection is left untreated, it can cause pain or lead to an abscess.
Who performs endodontic treatment?
All dentists, including your general dentist, receive basic training in endodontic treatment in dental school. General dentists often refer patients needing more specialized endodontic treatment to an endodontist. An endodontist is a dentist with special training in diagnosing and treating problems associated with the inside of the tooth.
What is endodontics?
Endodontics (Root Canal) therapy is a branch of dentistry recognized by the American Dental Association involving treatment of the pulp (root canal) and surrounding tissues of the tooth. When you look at your tooth in the mirror, what you see is the crown. The rest of the tooth, the portion hidden beneath the gum line, is called the root. Though the outer portion of the root is a hard tissue called dentin, the inside channel or “root canal” contains a pulp of soft tissue, blood vessels and nerves. Bacteria that are introduced into the pulp as a result of tooth decay, periodontal disease, tooth fracture or other problems, can severely damage the pulp. When the pulp is damaged, an endodontic specialist removes the tissue to save the tooth and prevent further infection and inflammation. After successful endodontic treatment, the tooth continues to perform normally.
What is an endodontist?
An endodontist is a dentist with special training in diagnosing and treating problems associated with the inside of the tooth. They do only endodontic procedures in their practices because they are specialists. To become specialists, they complete dental school and an additional two or more years of advanced training in endodontics, one of the nine specialties recognized by the American Dental Association. They perform routine as well as very complex endodontic procedures, including retreatment of previous root canals that have not healed completely, as well as endodontic surgery. Endodontists are also experienced at finding the cause of oral and facial pain that has been difficult to diagnose.
The Specialty training allows an Endodontist to:
- deal with diseases of the dental pulp and supporting structures.
- diagnose facial pain and related problems. Your general dentist sometimes refers patients for consultation when the diagnosis is complicated or when treatment is more difficult than normal.
- treat traumatic injuries to the teeth resulting from sports injuries or accidents.
- manage pain and swelling resulting from infected teeth.
Why canʼt my general dentist perform the treatment?
All dentists receive basic training in root canal treatment in dental school. Although some general dentists perform root canal procedures, many refer their patients to endodontists. Endodontists have two or three years of specialized training beyond dental school in root canal treatment. Many have performed thousands of procedures and are familiar with all the potential complications that may arise. They have specialized training in the latest technology, including the use of the ultrasonic, apex locator, digital imaging, and the operating microscope. Endodontics is one of the nine specialties recognized by the American Dental Association. Because they limit their practice to endodontics, endodontists have lots of experience in handling difficult cases, such as teeth with narrow or blocked canals or unusual anatomy.
Endodontic Procedures
What is endodontic retreatment therapy?
With proper care, most teeth that have had root canal (endodontic) treatment can last as long as other natural teeth. In some cases, however, a tooth that has received endodontic treatment fails to heal. Occasionally, the tooth becomes painful or diseased months or even years after successful treatment. If your tooth has not healed or has developed new problems, you have a second chance. Another procedure, endodontic retreatment, may be able to save your tooth.
I’m worried about X-rays. Should I be?
The risks associated with radiation exposure from dental radiographs are very minimal. While x-rays will be necessary during your endodontic treatment, we use a system called computerized digital radiography. The radiation levels used by this system can be up to 90 percent lower than those of conventional dental x-ray systems.
What causes an endodontically treated tooth to need additional treatment?
New trauma, deep decay, or a loose, cracked or broken filling can cause new infection in your tooth. In some cases, the endodontist may discover additional very narrow or curved canals that could not be treated during the initial procedure.
Will I feel pain during or after the procedure?
Many endodontic procedures are performed to relieve the pain of toothaches caused by pulp inflammation or infection. With modern techniques and anesthetics, most patients report that they are comfortable during the procedure. For the first few days after treatment, your tooth may feel sensitive, especially if there was pain or infection before the procedure. Your tooth may also continue to feel slightly different from your other teeth for some time after your endodontic treatment is completed. This discomfort can be relieved with over-the-counter or prescription medications. Follow your endodontist’s instructions carefully. However, if you have severe pain or pressure or pain that lasts more than a few days, call your endodontist.
How does endodontic treatment save the tooth?
The endodontist removes the inflamed or infected pulp, carefully cleans and shapes the inside of the canal, then fills and seals the space. Afterwards, you will return to your dentist, who will place a crown or other restoration on the tooth to protect and restore it to full function. After restoration, the tooth continues to function like any other tooth.
What are the signs of needing endodontic treatment?
Signs to look for include pain, prolonged sensitivity to heat or cold, tenderness to touch and chewing, discoloration of the tooth, and swelling, drainage and tenderness in the lymph nodes as well as nearby bone and gingival tissues. Sometimes, however, there are no symptoms.
Why would I need an endodontic procedure?
Endodontic treatment is necessary when the pulp, the soft tissue inside the root canal, becomes inflamed or infected. The inflammation or infection can have a variety of causes: deep decay, repeated dental procedures on the tooth, or a crack or chip in the tooth. In addition, an injury to a tooth may cause pulp damage even if the tooth has no visible chips or cracks. If pulp inflammation or infection is left untreated, it can cause pain or lead to an abscess.
Can I drive myself home after my appointment?
Often you can, but you should ask our staff before your appointment so that you can make transportation arrangements if necessary.
What do I do once the root canal is finished?
After treatment you will want to follow up with your general dentist. For more detailed information on what to expect after your procedure please read our AFTER TREATMENT BASICS or POST-SURGICAL INSTRUCTIONS. And, as always, all patient’s will be given the doctor’s direct line to contact him with any questions, issues, or concerns.